Book an Appointment
Colorectal Cancer
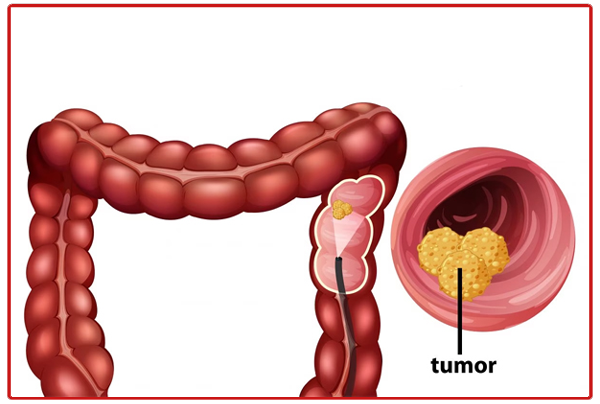
Colorectal Cancer
Overview;-
Colorectal cancer, also known as colon cancer or rectal cancer, is a type of cancer that develops in the colon or rectum. The colon and rectum are parts of the digestive system, with the colon being the large intestine and the rectum being the lower part of the colon that connects to the anus. Polyps (growths) in the inner lining of your colon cause colon cancer to form. Precancerous polyps can be found and removed using screening tests and therapies available to healthcare professionals. Colon cancer can spread to other parts of your body if it is not treated. Fewer individuals are passing away from colon cancer as a result of these tests, early diagnosis, and innovative types of therapy. The lengthy tube that assists in moving digested food to your rectum and out of your body, the colon (large intestine), is where colon (colorectal) cancer first appears. Layers of mucous membrane, tissue, and muscle make up your intestinal wall. The mucosa, or innermost lining of your colon, is where colon cancer first develops. It is made up of cells that produce and secrete fluids, including mucus. These cells have the potential to alter or mutate and become a colon polyp. Colon polyps might develop into cancer in the future. (A colon polyp develops cancer after around 10 years, on average.) The cancer spreads through a layer of tissue, muscle, and the outer layer of your colon if it is not discovered and/or treated. Your lymph nodes or blood arteries may allow the colon cancer to spread to other places in your body.
Symptoms:-
Colon cancer can exist without showing any signs of it. Even if you experience symptoms, you might not be able to tell if physical changes are indications of colon cancer. This is true because certain colon cancer symptoms are also present in other, less dangerous diseases. The following are typical signs of colon cancer:
- Constipation, diarrhea, or a change in the stool's consistency that lasts for a long time are examples of persistent changes in bowel habits.
- Bleeding from the rectum or blood in the stools
- Ongoing abdominal discomfort that includes cramps, gas, or pain
- A sensation that your bowels aren't totally emptied
- Weakness or exhaustion
- Unaccounted-for weight loss
Early on in the illness, colon cancer is often symptomless in many patients. Depending on the size and location of the cancer in your large intestine, symptoms may differ when they do.
Causes:-
Most colon cancers are unknown causes, according to doctors. Colon cancer often starts when normal colonic cells experience DNA abnormalities (mutations). A collection of instructions that inform a cell what to perform may be found in its DNA. Your body's healthy cells divide and develop in an organized fashion to maintain regular physiological function. However, when a cell's DNA is harmed and it becomes cancerous, it continues to divide even when new cells are not required. A tumor is created when the cells assemble. The cancer cells may spread over time and engulf neighboring healthy tissue, causing it to be destroyed. Additionally, malignant cells have the ability to spread to other areas of the body and deposit there (metastasize).
- Age: Colorectal cancer is more common in older adults, with the majority of cases occurring after the age of 50.
- Family history: Having a close relative, such as a parent or sibling, with colorectal cancer increases the risk.
- Personal history of polyps or colorectal cancer: Previous cases of colorectal cancer or certain types of polyps called adenomas can increase the risk.
- Inflammatory bowel disease (IBD): Chronic conditions like ulcerative colitis or Crohn's disease can increase the risk of developing colorectal cancer.
- Certain inherited genetic conditions: Conditions like familial adenomatous polyposis (FAP) or Lynch syndrome (hereditary nonpolyposis colorectal cancer) can significantly increase the risk.
Diagnosis:
Diagnosing colorectal cancer typically involves several steps, including:
- Screening tests: These tests, such as colonoscopy, are used to detect polyps or abnormal growths in the colon or rectum that could be precursors to cancer.
- Biopsy: If suspicious growths are found, a small sample of tissue is taken for examination under a microscope to determine if cancer is present.
- Imaging tests: Additional tests like CT scans, MRI, or PET scans may be used to determine the extent of cancer and check if it has spread to other parts of the body.
Treatment for colorectal cancer depends on the stage of the disease and other individual factors. It may include surgery, radiation therapy, chemotherapy, targeted therapy, immunotherapy, or a combination of these approaches. The goal of treatment is to remove the cancer, prevent its recurrence, or manage symptoms in advanced cases.
Treatment:
The ideal course of action for treating colorectal cancer relies on a number of variables. These consist of:
- the size and location of tumors and the cancer’s stage
- Whether the cancer is recurrent
- the person’s overall health
Surgery, radiation treatment, and chemotherapy are available options. Palliative care can also enhance quality of life while managing symptoms like pain.
For colorectal cancer that just affects the colon, surgery is the main course of therapy. In order to stop the disease from spreading, it removes malignant tissue, including tumors and damaged lymph nodes.
After removing malignant tissue, the surgeon often reconnects the intestine, although they might need to make a stoma for drainage into a colostomy bag. Usually, this is just transitory.
Early-stage cancer may be completely eradicated with surgery. Surgery cannot stop the cancer from progressing in its advanced stages, although clearing a blockage can assist with symptoms.
An extensive incision may be required during open surgery for colon cancer. It may be a laparoscopic procedure instead, which calls for very small incisions and is less intrusive. During surgery, the surgeon frequently employs robotic technology.
Prevention:
While it may not be possible to prevent colorectal cancer entirely, certain lifestyle changes and screenings can help reduce the risk or detect the disease at an early stage:
- Regular screenings: Recommended screening tests include colonoscopy, flexible sigmoidoscopy, and stool tests like fecal occult blood tests (FOBT) or fecal immunochemical tests (FIT).
- Healthy diet: A diet rich in fruits, vegetables, and whole grains, and low in red and processed meats can lower the risk.
- Physical activity: Regular exercise is associated with a reduced risk of colorectal cancer.
- Limit alcohol consumption.
- Avoid tobacco use.
- Maintain a healthy weight.
It's important to consult with a healthcare professional for personalized advice and guidance regarding screening and preventive measures based on individual risk factors. Healthcare professionals are now better equipped to detect and treat colon cancer before it spreads and produces symptoms because more patients are scheduling colon cancer screenings. More than 90% of those treated for early-stage colon cancer were still living five years after diagnosis, according to recent statistics on survival rates. Newer cancer-focused medicines help people with colon cancer as well. Ask your doctor whether there are any newer therapies that could be suitable for you if you have colon cancer.
Get In Touch
Tags
- Robotic Cancer Surgeon
- Laparoscopic Cancer Surgeon
- Dr. Tushar Aeron
- Dr. Tushar Aeron Dwarka
- Dr. Tushar Aeron Robotic Cancer Surgeon
- Dr. Tushar Aeron Laparoscopic Cancer Surgeon
- Robotic GI Surgeon
- Dr. Tushar Aeron Robotic GI Surgeon
- Dr. Tushar Aeron Robotic GI Surgeon Dwarka
- Best Oncologist in Dwarka Sector 18
- Best Oncosurgeon in Dwarka Sector 18
- best gastro surgeon in Dwarka sector 18
- Best Robotic Surgeon in Dwarka sector 18
- Best Laparoscopic Surgeon in Dwarka Sector 18
- best Gallbladder Surgery in Dwarka Sector 18
- liver transplant surgeon in Dwarka Sector 18
- Best liver transplant surgeon in Dwarka Sector 18
- best robotic cancer surgeon in Dwarka Sector 18
- best laparoscopic cancer surgeon in Dwarka Sector 18
- best surgical gastroenterologist in Dwarka Sector 18
- best GI Surgery Specialist in Dwarka Sector 18
- GI Surgery Specialist in Dwarka Sector 18
- Chronic Pancreatitis Treatment Specialist in Dwarka Sector 18
- Surgeon for GI Surgery in Dwarka Sector 18
- Surgeon for sleeve gastrectomy in Dwarka Sector 18
- Gallbladder Removal Surgeon in Dwarka Sector 18
- Best Gallbladder Removal Surgeon in Dwarka Sector 18
- Gallbladder Removal Surgery in Dwarka Sector 18
- Pancreato Biliary Surgery in Dwarka Sector 18
- Thoracoscopic Esophageal Surgery in Dwarka Sector 18
- Laparoscopic Colorectal Surgery in Dwarka Sector 18
- Best Oncologist in Dwarka
- Best Oncosurgeon in Dwarka
- best gastro surgeon in Dwarka
- Best Robotic Surgeon in Dwarka
- Best Laparoscopic Surgeon in Dwarka
- best Gallbladder Surgery in Dwarka
- liver transplant surgeon in Dwarka
- Best liver transplant surgeon in Dwarka
- best robotic cancer surgeon in Dwarka
- best laparoscopic cancer surgeon in Dwarka
- best surgical gastroenterologist in Dwarka
- best GI Surgery Specialist in Dwarka
- GI Surgery Specialist in Dwarka
- Chronic Pancreatitis Treatment Specialist in Dwarka
- Surgeon for GI Surgery in Dwarka
- Surgeon for sleeve gastrectomy in Dwarka
- Gallbladder Removal Surgeon in Dwarka
- Best Gallbladder Removal Surgeon in Dwarka
- Gallbladder Removal Surgery in Dwarka
- Pancreato Biliary Surgery in Dwarka
- Thoracoscopic Esophageal Surgery in Dwarka
- Laparoscopic Colorectal Surgery in Dwarka
- Best Oncologist in Janakpuri
- Best Oncosurgeon in Janakpuri
- best gastro surgeon in Janakpuri
- Best Robotic Surgeon in Janakpuri
- Best Laparoscopic Surgeon in Janakpuri
- best Gallbladder Surgery in Janakpuri
- liver transplant surgeon in Janakpuri
- Best liver transplant surgeon in Janakpuri
- best robotic cancer surgeon in Janakpuri
- best laparoscopic cancer surgeon in Janakpuri
- best surgical gastroenterologist in Janakpuri
- best GI Surgery Specialist in Janakpuri
- GI Surgery Specialist in Janakpuri
- Chronic Pancreatitis Treatment Specialist in Janakpuri
- Surgeon for GI Surgery in Janakpuri
- Surgeon for sleeve gastrectomy in Janakpuri
- Gallbladder Removal Surgeon in Janakpuri
- Best Gallbladder Removal Surgeon in Janakpuri
- Gallbladder Removal Surgery in Janakpuri
- Pancreato Biliary Surgery in Janakpuri
- Thoracoscopic Esophageal Surgery in Janakpuri
- Laparoscopic Colorectal Surgery in Janakpuri
- Best Oncologist in Palam
- Best Oncosurgeon in Palam
- best gastro surgeon in Palam
- Best Robotic Surgeon in Palam
- Best Laparoscopic Surgeon in Palam
- best Gallbladder Surgery in Palam
- liver transplant surgeon in Palam
- Best liver transplant surgeon in Palam
- best robotic cancer surgeon in Palam
- best laparoscopic cancer surgeon in Palam
- best surgical gastroenterologist in Palam
- best GI Surgery Specialist in Palam
- GI Surgery Specialist in Palam
- Chronic Pancreatitis Treatment Specialist in Palam
- Surgeon for GI Surgery in Palam
- Surgeon for sleeve gastrectomy in Palam
- Gallbladder Removal Surgeon in Palam
- Best Gallbladder Removal Surgeon in Palam
- Gallbladder Removal Surgery in Palam
- Pancreato Biliary Surgery in Palam
- Thoracoscopic Esophageal Surgery in Palam
- Laparoscopic Colorectal Surgery in Palam
- Best Oncologist in Najafgarh
- Best Oncosurgeon in Najafgarh
- best gastro surgeon in Najafgarh
- Best Robotic Surgeon in Najafgarh
- Best Laparoscopic Surgeon in Najafgarh
- best Gallbladder Surgery in Najafgarh
- liver transplant surgeon in Najafgarh
- Best liver transplant surgeon in Najafgarh
- best robotic cancer surgeon in Najafgarh
- best laparoscopic cancer surgeon in Najafgarh
- best surgical gastroenterologist in Najafgarh
- best GI Surgery Specialist in Najafgarh
- GI Surgery Specialist in Najafgarh
- Chronic Pancreatitis Treatment Specialist in Najafgarh
- Surgeon for GI Surgery in Najafgarh
- Surgeon for sleeve gastrectomy in Najafgarh
- Gallbladder Removal Surgeon in Najafgarh
- Best Gallbladder Removal Surgeon in Najafgarh
- Gallbladder Removal Surgery in Najafgarh
- Pancreato Biliary Surgery in Najafgarh
- Thoracoscopic Esophageal Surgery in Najafgarh
- Laparoscopic Colorectal Surgery in Najafgarh
- Best Oncologist in Dwarka Sector 19
- Best Oncosurgeon in Dwarka Sector 19
- best gastro surgeon in Dwarka Sector 19
- Best Robotic Surgeon in Dwarka Sector 19
- Best Laparoscopic Surgeon in Dwarka Sector 19
- best Gallbladder Surgery in Dwarka Sector 19
- liver transplant surgeon in Dwarka Sector 19
- Best liver transplant surgeon in Dwarka Sector 19
- best robotic cancer surgeon in Dwarka Sector 19
- best laparoscopic cancer surgeon in Dwarka Sector 19
- best surgical gastroenterologist in Dwarka Sector 19
- best GI Surgery Specialist in Dwarka Sector 19
- GI Surgery Specialist in Dwarka Sector 19
- Chronic Pancreatitis Treatment Specialist in Dwarka Sector 19
- Surgeon for GI Surgery in Dwarka Sector 19
- Surgeon for sleeve gastrectomy in Dwarka Sector 19
- Gallbladder Removal Surgeon in Dwarka Sector 19
- Best Gallbladder Removal Surgeon in Dwarka Sector 19
- Gallbladder Removal Surgery in Dwarka Sector 19
- Pancreato Biliary Surgery in Dwarka Sector 19
- Thoracoscopic Esophageal Surgery in Dwarka Sector 19
- Laparoscopic Colorectal Surgery in Dwarka Sector 19
- Best Oncologist in Dwarka Sector 20
- Best Oncosurgeon in Dwarka Sector 20
- best gastro surgeon in Dwarka Sector 20
- Best Robotic Surgeon in Dwarka Sector 20
- Best Laparoscopic Surgeon in Dwarka Sector 20
- best Gallbladder Surgery in Dwarka Sector 20
- liver transplant surgeon in Dwarka Sector 20
- Best liver transplant surgeon in Dwarka Sector 20
- best robotic cancer surgeon in Dwarka Sector 20
- best laparoscopic cancer surgeon in Dwarka Sector 20
- best surgical gastroenterologist in Dwarka Sector 20
- best GI Surgery Specialist in Dwarka Sector 20
- GI Surgery Specialist in Dwarka Sector 20
- Chronic Pancreatitis Treatment Specialist in Dwarka Sector 20
- Surgeon for GI Surgery in Dwarka Sector 20
- Surgeon for sleeve gastrectomy in Dwarka Sector 20
- Gallbladder Removal Surgeon in Dwarka Sector 20
- Best Gallbladder Removal Surgeon in Dwarka Sector 20
- Gallbladder Removal Surgery in Dwarka Sector 20
- Pancreato Biliary Surgery in Dwarka Sector 20
- Thoracoscopic Esophageal Surgery in Dwarka Sector 20
- Laparoscopic Colorectal Surgery in Dwarka Sector 20
- Best Oncologist in Dwarka Sector 21
- Best Oncosurgeon in Dwarka Sector 21
- best gastro surgeon in Dwarka Sector 21
- Best Robotic Surgeon in Dwarka Sector 21
- Best Laparoscopic Surgeon in Dwarka Sector 21
- best Gallbladder Surgery in Dwarka Sector 21
- liver transplant surgeon in Dwarka Sector 21
- Best liver transplant surgeon in Dwarka Sector 21
- best robotic cancer surgeon in Dwarka Sector 21
- best laparoscopic cancer surgeon in Dwarka Sector 21
- best surgical gastroenterologist in Dwarka Sector 21
- best GI Surgery Specialist in Dwarka Sector 21
- GI Surgery Specialist in Dwarka Sector 21
- Chronic Pancreatitis Treatment Specialist in Dwarka Sector 21
- Surgeon for GI Surgery in Dwarka Sector 21
- Surgeon for sleeve gastrectomy in Dwarka Sector 21
- Gallbladder Removal Surgeon in Dwarka Sector 21
- Best Gallbladder Removal Surgeon in Dwarka Sector 21
- Gallbladder Removal Surgery in Dwarka Sector 21
- Pancreato Biliary Surgery in Dwarka Sector 21
- Thoracoscopic Esophageal Surgery in Dwarka Sector 21
- Laparoscopic Colorectal Surgery in Dwarka Sector 21
- Best Oncologist in Dwarka Sector 17
- Best Oncosurgeon in Dwarka Sector 17
- best gastro surgeon in Dwarka Sector 17
- Best Robotic Surgeon in Dwarka Sector 17
- Best Laparoscopic Surgeon in Dwarka Sector 17
- best Gallbladder Surgery in Dwarka Sector 17
- liver transplant surgeon in Dwarka Sector 17
- Best liver transplant surgeon in Dwarka Sector 17
- best robotic cancer surgeon in Dwarka Sector 17
- best laparoscopic cancer surgeon in Dwarka Sector 17
- best surgical gastroenterologist in Dwarka Sector 17
- best GI Surgery Specialist in Dwarka Sector 17
- GI Surgery Specialist in Dwarka Sector 17
- Chronic Pancreatitis Treatment Specialist in Dwarka Sector 17
- Surgeon for GI Surgery in Dwarka Sector 17
- Surgeon for sleeve gastrectomy in Dwarka Sector 17
- Gallbladder Removal Surgeon in Dwarka Sector 17
- Best Gallbladder Removal Surgeon in Dwarka Sector 17
- Gallbladder Removal Surgery in Dwarka Sector 17
- Pancreato Biliary Surgery in Dwarka Sector 17
- Thoracoscopic Esophageal Surgery in Dwarka Sector 17
- Laparoscopic Colorectal Surgery in Dwarka Sector 17
- Best Oncologist in Dwarka Sector 16
- Best Oncosurgeon in Dwarka Sector 16
- best gastro surgeon in Dwarka Sector 16
- Best Robotic Surgeon in Dwarka Sector 16
- Best Laparoscopic Surgeon in Dwarka Sector 16
- best Gallbladder Surgery in Dwarka Sector 16
- liver transplant surgeon in Dwarka Sector 16
- Best liver transplant surgeon in Dwarka Sector 16
- best robotic cancer surgeon in Dwarka Sector 16
- best laparoscopic cancer surgeon in Dwarka Sector 16
- best surgical gastroenterologist in Dwarka Sector 16
- best GI Surgery Specialist in Dwarka Sector 16
- GI Surgery Specialist in Dwarka Sector 16
- Chronic Pancreatitis Treatment Specialist in Dwarka Sector 16
- Surgeon for GI Surgery in Dwarka Sector 16
- Surgeon for sleeve gastrectomy in Dwarka Sector 16
- Gallbladder Removal Surgeon in Dwarka Sector 16
- Best Gallbladder Removal Surgeon in Dwarka Sector 16
- Gallbladder Removal Surgery in Dwarka Sector 16
- Pancreato Biliary Surgery in Dwarka Sector 16
- Thoracoscopic Esophageal Surgery in Dwarka Sector 16
- Laparoscopic Colorectal Surgery in Dwarka Sector 16
- Best Oncologist in Dwarka Sector 15
- Best Oncosurgeon in Dwarka Sector 15
- best gastro surgeon in Dwarka Sector 15
- Best Robotic Surgeon in Dwarka Sector 15
- Best Laparoscopic Surgeon in Dwarka Sector 15
- best Gallbladder Surgery in Dwarka Sector 15
- liver transplant surgeon in Dwarka Sector 15
- Best liver transplant surgeon in Dwarka Sector 15
- best robotic cancer surgeon in Dwarka Sector 15
- best laparoscopic cancer surgeon in Dwarka Sector 15
- best surgical gastroenterologist in Dwarka Sector 15
- best GI Surgery Specialist in Dwarka Sector 15
- GI Surgery Specialist in Dwarka Sector 15
- Chronic Pancreatitis Treatment Specialist in Dwarka Sector 15
- Surgeon for GI Surgery in Dwarka Sector 15
- Surgeon for sleeve gastrectomy in Dwarka Sector 15
- Gallbladder Removal Surgeon in Dwarka Sector 15
- Best Gallbladder Removal Surgeon in Dwarka Sector 15
- Gallbladder Removal Surgery in Dwarka Sector 15
- Pancreato Biliary Surgery in Dwarka Sector 15
- Thoracoscopic Esophageal Surgery in Dwarka Sector 15
- Laparoscopic Colorectal Surgery in Dwarka Sector 15
- Best Oncologist in Dwarka Sector 14
- Best Oncosurgeon in Dwarka Sector 14
- best gastro surgeon in Dwarka Sector 14
- Best Robotic Surgeon in Dwarka Sector 14
- Best Laparoscopic Surgeon in Dwarka Sector 14
- best Gallbladder Surgery in Dwarka Sector 14
- liver transplant surgeon in Dwarka Sector 14
- Best liver transplant surgeon in Dwarka Sector 14
- best robotic cancer surgeon in Dwarka Sector 14
- best laparoscopic cancer surgeon in Dwarka Sector 14
- best surgical gastroenterologist in Dwarka Sector 14
- best GI Surgery Specialist in Dwarka Sector 14
- GI Surgery Specialist in Dwarka Sector 14
- Chronic Pancreatitis Treatment Specialist in Dwarka Sector 14
- Surgeon for GI Surgery in Dwarka Sector 14
- Surgeon for sleeve gastrectomy in Dwarka Sector 14
- Gallbladder Removal Surgeon in Dwarka Sector 14
- Best Gallbladder Removal Surgeon in Dwarka Sector 14
- Gallbladder Removal Surgery in Dwarka Sector 14
- Pancreato Biliary Surgery in Dwarka Sector 14
- Thoracoscopic Esophageal Surgery in Dwarka Sector 14
- Laparoscopic Colorectal Surgery in Dwarka Sector 14
- Best Oncologist in Dwarka Sector 1
- Best Oncosurgeon in Dwarka Sector 1
- best gastro surgeon in Dwarka Sector 1
- Best Robotic Surgeon in Dwarka Sector 1
- Best Laparoscopic Surgeon in Dwarka Sector 1
- best Gallbladder Surgery in Dwarka Sector 1
- liver transplant surgeon in Dwarka Sector 1
- Best liver transplant surgeon in Dwarka Sector 1
- best robotic cancer surgeon in Dwarka Sector 1
- best laparoscopic cancer surgeon in Dwarka Sector 1
- best surgical gastroenterologist in Dwarka Sector 1
- best GI Surgery Specialist in Dwarka Sector 1
- GI Surgery Specialist in Dwarka Sector 1
- Chronic Pancreatitis Treatment Specialist in Dwarka Sector 1
- Surgeon for GI Surgery in Dwarka Sector 1
- Surgeon for sleeve gastrectomy in Dwarka Sector 1
- Gallbladder Removal Surgeon in Dwarka Sector 1
- Best Gallbladder Removal Surgeon in Dwarka Sector 1
- Gallbladder Removal Surgery in Dwarka Sector 1
- Pancreato Biliary Surgery in Dwarka Sector 1
- Thoracoscopic Esophageal Surgery in Dwarka Sector 1
- Laparoscopic Colorectal Surgery in Dwarka Sector 1
- Best Oncologist in Dwarka Sector 2
- Best Oncosurgeon in Dwarka Sector 2
- best gastro surgeon in Dwarka Sector 2
- Best Robotic Surgeon in Dwarka Sector 2
- Best Laparoscopic Surgeon in Dwarka Sector 2
- best Gallbladder Surgery in Dwarka Sector 2
- liver transplant surgeon in Dwarka Sector 2
- Best liver transplant surgeon in Dwarka Sector 2
- best robotic cancer surgeon in Dwarka Sector 2
- best laparoscopic cancer surgeon in Dwarka Sector 2
- best surgical gastroenterologist in Dwarka Sector 2
- best GI Surgery Specialist in Dwarka Sector 2
- GI Surgery Specialist in Dwarka Sector 2
- Chronic Pancreatitis Treatment Specialist in Dwarka Sector 2
- Surgeon for GI Surgery in Dwarka Sector 2
- Surgeon for sleeve gastrectomy in Dwarka Sector 2
- Gallbladder Removal Surgeon in Dwarka Sector 2
- Best Gallbladder Removal Surgeon in Dwarka Sector 2
- Gallbladder Removal Surgery in Dwarka Sector 2
- Pancreato Biliary Surgery in Dwarka Sector 2
- Thoracoscopic Esophageal Surgery in Dwarka Sector 2
- Laparoscopic Colorectal Surgery in Dwarka Sector 2
- Best Oncologist in Dwarka Sector 3
- Best Oncosurgeon in Dwarka Sector 3
- best gastro surgeon in Dwarka Sector 3
- Best Robotic Surgeon in Dwarka Sector 3
- Best Laparoscopic Surgeon in Dwarka Sector 3
- best Gallbladder Surgery in Dwarka Sector 3
- liver transplant surgeon in Dwarka Sector 3
- Best liver transplant surgeon in Dwarka Sector 3
- best robotic cancer surgeon in Dwarka Sector 3
- best laparoscopic cancer surgeon in Dwarka Sector 3
- best surgical gastroenterologist in Dwarka Sector 3
- best GI Surgery Specialist in Dwarka Sector 3
- GI Surgery Specialist in Dwarka Sector 3
- Chronic Pancreatitis Treatment Specialist in Dwarka Sector 3
- Surgeon for GI Surgery in Dwarka Sector 3
- Surgeon for sleeve gastrectomy in Dwarka Sector 3
- Gallbladder Removal Surgeon in Dwarka Sector 3
- Best Gallbladder Removal Surgeon in Dwarka Sector 3
- Gallbladder Removal Surgery in Dwarka Sector 3
- Pancreato Biliary Surgery in Dwarka Sector 3
- Thoracoscopic Esophageal Surgery in Dwarka Sector 3
- Laparoscopic Colorectal Surgery in Dwarka Sector 3
- Best Oncologist in Dwarka Sector 4
- Best Oncosurgeon in Dwarka Sector 4
- best gastro surgeon in Dwarka Sector 4
- Best Robotic Surgeon in Dwarka Sector 4
- Best Laparoscopic Surgeon in Dwarka Sector 4
- best Gallbladder Surgery in Dwarka Sector 4
- liver transplant surgeon in Dwarka Sector 4
- Best liver transplant surgeon in Dwarka Sector 4
- best robotic cancer surgeon in Dwarka Sector 4
- best laparoscopic cancer surgeon in Dwarka Sector 4
- best surgical gastroenterologist in Dwarka Sector 4
- best GI Surgery Specialist in Dwarka Sector 4
- GI Surgery Specialist in Dwarka Sector 4
- Chronic Pancreatitis Treatment Specialist in Dwarka Sector 4
- Surgeon for GI Surgery in Dwarka Sector 4
- Surgeon for sleeve gastrectomy in Dwarka Sector 4
- Gallbladder Removal Surgeon in Dwarka Sector 4
- Best Gallbladder Removal Surgeon in Dwarka Sector 4
- Gallbladder Removal Surgery in Dwarka Sector 4
- Pancreato Biliary Surgery in Dwarka Sector 4
- Thoracoscopic Esophageal Surgery in Dwarka Sector 4
- Laparoscopic Colorectal Surgery in Dwarka Sector 4
- Best Oncologist in Dwarka Sector 5
- Best Oncosurgeon in Dwarka Sector 5
- best gastro surgeon in Dwarka Sector 5
- Best Robotic Surgeon in Dwarka Sector 5
- Best Laparoscopic Surgeon in Dwarka Sector 5
- best Gallbladder Surgery in Dwarka Sector 5
- liver transplant surgeon in Dwarka Sector 5
- Best liver transplant surgeon in Dwarka Sector 5
- best robotic cancer surgeon in Dwarka Sector 5
- best laparoscopic cancer surgeon in Dwarka Sector 5
- best surgical gastroenterologist in Dwarka Sector 5
- best GI Surgery Specialist in Dwarka Sector 5
- GI Surgery Specialist in Dwarka Sector 5
- Chronic Pancreatitis Treatment Specialist in Dwarka Sector 5
- Surgeon for GI Surgery in Dwarka Sector 5
- Surgeon for sleeve gastrectomy in Dwarka Sector 5
- Gallbladder Removal Surgeon in Dwarka Sector 5
- Best Gallbladder Removal Surgeon in Dwarka Sector 5
- Gallbladder Removal Surgery in Dwarka Sector 5
- Pancreato Biliary Surgery in Dwarka Sector 5
- Thoracoscopic Esophageal Surgery in Dwarka Sector 5
- Laparoscopic Colorectal Surgery in Dwarka Sector 5
- Best Oncologist in Dwarka Sector 6
- Best Oncosurgeon in Dwarka Sector 6
- best gastro surgeon in Dwarka Sector 6
- Best Robotic Surgeon in Dwarka Sector 6
- Best Laparoscopic Surgeon in Dwarka Sector 6
- best Gallbladder Surgery in Dwarka Sector 6
- liver transplant surgeon in Dwarka Sector 6
- Best liver transplant surgeon in Dwarka Sector 6
- best robotic cancer surgeon in Dwarka Sector 6
- best laparoscopic cancer surgeon in Dwarka Sector 6
- best surgical gastroenterologist in Dwarka Sector 6
- best GI Surgery Specialist in Dwarka Sector 6
- GI Surgery Specialist in Dwarka Sector 6
- Chronic Pancreatitis Treatment Specialist in Dwarka Sector 6
- Surgeon for GI Surgery in Dwarka Sector 6
- Surgeon for sleeve gastrectomy in Dwarka Sector 6
- Gallbladder Removal Surgeon in Dwarka Sector 6
- Best Gallbladder Removal Surgeon in Dwarka Sector 6
- Gallbladder Removal Surgery in Dwarka Sector 6
- Pancreato Biliary Surgery in Dwarka Sector 6
- Thoracoscopic Esophageal Surgery in Dwarka Sector 6
- Laparoscopic Colorectal Surgery in Dwarka Sector 6
- Best Oncologist in Dwarka Sector 7
- Best Oncosurgeon in Dwarka Sector 7
- best gastro surgeon in Dwarka Sector 7
- Best Robotic Surgeon in Dwarka Sector 7
- Best Laparoscopic Surgeon in Dwarka Sector 7
- best Gallbladder Surgery in Dwarka Sector 7
- liver transplant surgeon in Dwarka Sector 7
- Best liver transplant surgeon in Dwarka Sector 7
- best robotic cancer surgeon in Dwarka Sector 7
- best laparoscopic cancer surgeon in Dwarka Sector 7
- best surgical gastroenterologist in Dwarka Sector 7
- best GI Surgery Specialist in Dwarka Sector 7
- GI Surgery Specialist in Dwarka Sector 7
- Chronic Pancreatitis Treatment Specialist in Dwarka Sector 7
- Surgeon for GI Surgery in Dwarka Sector 7
- Surgeon for sleeve gastrectomy in Dwarka Sector 7
- Gallbladder Removal Surgeon in Dwarka Sector 7
- Best Gallbladder Removal Surgeon in Dwarka Sector 7
- Gallbladder Removal Surgery in Dwarka Sector 7
- Pancreato Biliary Surgery in Dwarka Sector 7
- Thoracoscopic Esophageal Surgery in Dwarka Sector 7
- Laparoscopic Colorectal Surgery in Dwarka Sector 7
- Best Oncologist in Dwarka Sector 8
- Best Oncosurgeon in Dwarka Sector 8
- best gastro surgeon in Dwarka Sector 8
- Best Robotic Surgeon in Dwarka Sector 8
- Best Laparoscopic Surgeon in Dwarka Sector 8
- best Gallbladder Surgery in Dwarka Sector 8
- liver transplant surgeon in Dwarka Sector 8
- Best liver transplant surgeon in Dwarka Sector 8
- best robotic cancer surgeon in Dwarka Sector 8
- best laparoscopic cancer surgeon in Dwarka Sector 8
- best surgical gastroenterologist in Dwarka Sector 8
- best GI Surgery Specialist in Dwarka Sector 8
- GI Surgery Specialist in Dwarka Sector 8
- Chronic Pancreatitis Treatment Specialist in Dwarka Sector 8
- Surgeon for GI Surgery in Dwarka Sector 8
- Surgeon for sleeve gastrectomy in Dwarka Sector 8
- Gallbladder Removal Surgeon in Dwarka Sector 8
- Best Gallbladder Removal Surgeon in Dwarka Sector 8
- Gallbladder Removal Surgery in Dwarka Sector 8
- Pancreato Biliary Surgery in Dwarka Sector 8
- Thoracoscopic Esophageal Surgery in Dwarka Sector 8
- Laparoscopic Colorectal Surgery in Dwarka Sector 8
- Best Oncologist in Dwarka Sector 9
- Best Oncosurgeon in Dwarka Sector 9
- best gastro surgeon in Dwarka Sector 9
- Best Robotic Surgeon in Dwarka Sector 9
- Best Laparoscopic Surgeon in Dwarka Sector 9
- best Gallbladder Surgery in Dwarka Sector 9
- liver transplant surgeon in Dwarka Sector 9
- Best liver transplant surgeon in Dwarka Sector 9
- best robotic cancer surgeon in Dwarka Sector 9
- best laparoscopic cancer surgeon in Dwarka Sector 9
- best surgical gastroenterologist in Dwarka Sector 9
- best GI Surgery Specialist in Dwarka Sector 9
- GI Surgery Specialist in Dwarka Sector 9
- Chronic Pancreatitis Treatment Specialist in Dwarka Sector 9
- Surgeon for GI Surgery in Dwarka Sector 9
- Surgeon for sleeve gastrectomy in Dwarka Sector 9
- Gallbladder Removal Surgeon in Dwarka Sector 9
- Best Gallbladder Removal Surgeon in Dwarka Sector 9
- Gallbladder Removal Surgery in Dwarka Sector 9
- Pancreato Biliary Surgery in Dwarka Sector 9
- Thoracoscopic Esophageal Surgery in Dwarka Sector 9
- Laparoscopic Colorectal Surgery in Dwarka Sector 9
- Best Oncologist in Dwarka Sector 10
- Best Oncosurgeon in Dwarka Sector 10
- best gastro surgeon in Dwarka Sector 10
- Best Robotic Surgeon in Dwarka Sector 10
- Best Laparoscopic Surgeon in Dwarka Sector 10
- best Gallbladder Surgery in Dwarka Sector 10
- liver transplant surgeon in Dwarka Sector 10
- Best liver transplant surgeon in Dwarka Sector 10
- best robotic cancer surgeon in Dwarka Sector 10
- best laparoscopic cancer surgeon in Dwarka Sector 10
- best surgical gastroenterologist in Dwarka Sector 10
- best GI Surgery Specialist in Dwarka Sector 10
- GI Surgery Specialist in Dwarka Sector 10
- Chronic Pancreatitis Treatment Specialist in Dwarka Sector 10
- Surgeon for GI Surgery in Dwarka Sector 10
- Surgeon for sleeve gastrectomy in Dwarka Sector 10
- Gallbladder Removal Surgeon in Dwarka Sector 10
- Best Gallbladder Removal Surgeon in Dwarka Sector 10
- Gallbladder Removal Surgery in Dwarka Sector 10
- Pancreato Biliary Surgery in Dwarka Sector 10
- Thoracoscopic Esophageal Surgery in Dwarka Sector 10
- Laparoscopic Colorectal Surgery in Dwarka Sector 10
- Best Oncologist in Ashok Vihar
- Best Oncosurgeon in Ashok Vihar
- best gastro surgeon in Ashok Vihar
- Best Robotic Surgeon in Ashok Vihar
- Best Laparoscopic Surgeon in Ashok Vihar
- best Gallbladder Surgery in Ashok Vihar
- liver transplant surgeon in Ashok Vihar
- Best liver transplant surgeon in Ashok Vihar
- best robotic cancer surgeon in Ashok Vihar
- best laparoscopic cancer surgeon in Ashok Vihar
- best surgical gastroenterologist in Ashok Vihar
- best GI Surgery Specialist in Ashok Vihar
- GI Surgery Specialist in Ashok Vihar
- Chronic Pancreatitis Treatment Specialist in Ashok Vihar
- Surgeon for GI Surgery in Ashok Vihar
- Surgeon for sleeve gastrectomy in Ashok Vihar
- Gallbladder Removal Surgeon in Ashok Vihar
- Best Gallbladder Removal Surgeon in Ashok Vihar
- Gallbladder Removal Surgery in Ashok Vihar
- Pancreato Biliary Surgery in Ashok Vihar
- Thoracoscopic Esophageal Surgery in Ashok Vihar
- Laparoscopic Colorectal Surgery in Ashok Vihar
- Best Oncologist in Shalimar Bagh
- Best Oncosurgeon in Shalimar Bagh
- best gastro surgeon in Shalimar Bagh
- Best Robotic Surgeon in Shalimar Bagh
- Best Laparoscopic Surgeon in Shalimar Bagh
- best Gallbladder Surgery in Shalimar Bagh
- liver transplant surgeon in Shalimar Bagh
- Best liver transplant surgeon in Shalimar Bagh
- best robotic cancer surgeon in Shalimar Bagh
- best laparoscopic cancer surgeon in Shalimar Bagh
- best surgical gastroenterologist in Shalimar Bagh
- best GI Surgery Specialist in Shalimar Bagh
- GI Surgery Specialist in Shalimar Bagh
- Chronic Pancreatitis Treatment Specialist in Shalimar Bagh
- Surgeon for GI Surgery in Shalimar Bagh
- Surgeon for sleeve gastrectomy in Shalimar Bagh
- Gallbladder Removal Surgeon in Shalimar Bagh
- Best Gallbladder Removal Surgeon in Shalimar Bagh
- Gallbladder Removal Surgery in Shalimar Bagh
- Pancreato Biliary Surgery in Shalimar Bagh
- Thoracoscopic Esophageal Surgery in Shalimar Bagh
- Laparoscopic Colorectal Surgery in Shalimar Bagh
- Best Oncologist in Rohini
- Best Oncosurgeon in Rohini
- best gastro surgeon in Rohini
- Best Robotic Surgeon in Rohini
- Best Laparoscopic Surgeon in Rohini
- best Gallbladder Surgery in Rohini
- liver transplant surgeon in Rohini
- Best liver transplant surgeon in Rohini
- best robotic cancer surgeon in Rohini
- best laparoscopic cancer surgeon in Rohini
- best surgical gastroenterologist in Rohini
- best GI Surgery Specialist in Rohini
- GI Surgery Specialist in Rohini
- Chronic Pancreatitis Treatment Specialist in Rohini
- Surgeon for GI Surgery in Rohini
- Surgeon for sleeve gastrectomy in Rohini
- Gallbladder Removal Surgeon in Rohini
- Best Gallbladder Removal Surgeon in Rohini
- Gallbladder Removal Surgery in Rohini
- Pancreato Biliary Surgery in Rohini
- Thoracoscopic Esophageal Surgery in Rohini
- Laparoscopic Colorectal Surgery in Rohini
- Best Oncologist in Karol Bagh
- Best Oncosurgeon in Karol Bagh
- best gastro surgeon in Karol Bagh
- Best Robotic Surgeon in Karol Bagh
- Best Laparoscopic Surgeon in Karol Bagh
- best Gallbladder Surgery in Karol Bagh
- liver transplant surgeon in Karol Bagh
- Best liver transplant surgeon in Karol Bagh
- best robotic cancer surgeon in Karol Bagh
- best laparoscopic cancer surgeon in Karol Bagh
- best surgical gastroenterologist in Karol Bagh
- best GI Surgery Specialist in Karol Bagh
- GI Surgery Specialist in Karol Bagh
- Chronic Pancreatitis Treatment Specialist in Karol Bagh
- Surgeon for GI Surgery in Karol Bagh
- Surgeon for sleeve gastrectomy in Karol Bagh
- Gallbladder Removal Surgeon in Karol Bagh
- Best Gallbladder Removal Surgeon in Karol Bagh
- Gallbladder Removal Surgery in Karol Bagh
- Pancreato Biliary Surgery in Karol Bagh
- Thoracoscopic Esophageal Surgery in Karol Bagh
- Laparoscopic Colorectal Surgery in Karol Bagh
- Best Oncologist in Pitampura
- Best Oncosurgeon in Pitampura
- best gastro surgeon in Pitampura
- Best Robotic Surgeon in Pitampura
- Best Laparoscopic Surgeon in Pitampura
- best Gallbladder Surgery in Pitampura
- liver transplant surgeon in Pitampura
- Best liver transplant surgeon in Pitampura
- best robotic cancer surgeon in Pitampura
- best laparoscopic cancer surgeon in Pitampura
- best surgical gastroenterologist in Pitampura
- best GI Surgery Specialist in Pitampura
- GI Surgery Specialist in Pitampura
- Chronic Pancreatitis Treatment Specialist in Pitampura
- Surgeon for GI Surgery in Pitampura
- Surgeon for sleeve gastrectomy in Pitampura
- Gallbladder Removal Surgeon in Pitampura
- Best Gallbladder Removal Surgeon in Pitampura
- Gallbladder Removal Surgery in Pitampura
- Pancreato Biliary Surgery in Pitampura
- Thoracoscopic Esophageal Surgery in Pitampura
- Laparoscopic Colorectal Surgery in Pitampura
- best Oncologist in Dwarka
- best oncosurgeon in Dwarka
- best onco surgeon in Dwarka
- best gastro doctor in Dwarka
- best gastrosurgeon in Dwarka
- best robotic surgeon in Dwarka
- best laparoscopic surgeon in Dwarka
- gallbladder surgery in Dwarka
- gall bladder surgery in Dwarka
- best Oncologist in Janakpuri
- best oncosurgeon in Janakpuri
- best onco surgeon in Janakpuri
- best gastro doctor in Janakpuri
- best gastrosurgeon in Janakpuri
- best robotic surgeon in Janakpuri
- best laparoscopic surgeon in Janakpuri
- gallbladder surgery in Janakpuri
- gall bladder surgery in Janakpuri
- best Oncologist in Palam
- best oncosurgeon in Palam
- best onco surgeon in Palam
- best gastro doctor in Palam
- best gastrosurgeon in Palam
- best robotic surgeon in Palam
- best laparoscopic surgeon in Palam
- gallbladder surgery in Palam
- gall bladder surgery in Palam
- best Oncologist in Najafgarh
- best oncosurgeon in Najafgarh
- best onco surgeon in Najafgarh
- best gastro doctor in Najafgarh
- best gastrosurgeon in Najafgarh
- best robotic surgeon in Najafgarh
- best laparoscopic surgeon in Najafgarh
- gallbladder surgery in Najafgarh
- gall bladder surgery in Najafgarh
- best Oncologist in Rajouri Garden
- best oncosurgeon in Rajouri Garden
- best onco surgeon in Rajouri Garden
- best gastro surgeon in Rajouri Garden
- best gastro doctor in Rajouri Garden
- best gastrosurgeon in Rajouri Garden
- best robotic surgeon in Rajouri Garden
- best robotic cancer surgeon in Rajouri Garden
- best laparoscopic surgeon in Rajouri Garden
- gallbladder surgery in Rajouri Garden
- gall bladder surgery in Rajouri Garden
- best Oncologist in Ashok Vihar
- best oncosurgeon in Ashok Vihar
- best onco surgeon in Ashok Vihar
- best gastro doctor in Ashok Vihar
- best gastrosurgeon in Ashok Vihar
- best robotic surgeon in Ashok Vihar
- best laparoscopic surgeon in Ashok Vihar
- gallbladder surgery in Ashok Vihar
- gall bladder surgery in Ashok Vihar
- best Oncologist in Shalimar Bagh
- best oncosurgeon in Shalimar Bagh
- best onco surgeon in Shalimar Bagh
- best gastro doctor in Shalimar Bagh
- best gastrosurgeon in Shalimar Bagh
- best robotic surgeon in Shalimar Bagh
- best laparoscopic surgeon in Shalimar Bagh
- gallbladder surgery in Shalimar Bagh
- gall bladder surgery in Shalimar Bagh
- best Oncologist in Rohini
- best oncosurgeon in Rohini
- best onco surgeon in Rohini
- best gastro doctor in Rohini
- best gastrosurgeon in Rohini
- best robotic surgeon in Rohini
- best laparoscopic surgeon in Rohini
- gallbladder surgery in Rohini
- gall bladder surgery in Rohini
- best Oncologist in Karol Bagh
- best oncosurgeon in Karol Bagh
- best onco surgeon in Karol Bagh
- best gastro doctor in Karol Bagh
- best gastrosurgeon in Karol Bagh
- best robotic surgeon in Karol Bagh
- best laparoscopic surgeon in Karol Bagh
- gallbladder surgery in Karol Bagh
- gall bladder surgery in Karol Bagh
- best Oncologist in Pitampura
- best oncosurgeon in Pitampura
- best onco surgeon in Pitampura
- best gastro doctor in Pitampura
- best gastrosurgeon in Pitampura
- best robotic surgeon in Pitampura
- best laparoscopic surgeon in Pitampura
- gallbladder surgery in Pitampura
- gall bladder surgery in Pitampura
- best Oncologist in Vikaspuri
- best oncosurgeon in Vikaspuri
- best onco surgeon in Vikaspuri
- best gastro surgeon in Vikaspuri
- best gastro doctor in Vikaspuri
- best gastrosurgeon in Vikaspuri
- best robotic surgeon in Vikaspuri
- best robotic cancer surgeon in Vikaspuri
- best laparoscopic surgeon in Vikaspuri
- gallbladder surgery in Vikaspuri
- gall bladder surgery in Vikaspuri
- best Oncologist in Uttam Nagar
- best oncosurgeon in Uttam Nagar
- best onco surgeon in Uttam Nagar
- best gastro surgeon in Uttam Nagar
- best gastro doctor in Uttam Nagar
- best gastrosurgeon in Uttam Nagar
- best robotic surgeon in Uttam Nagar
- best robotic cancer surgeon in Uttam Nagar
- best laparoscopic surgeon in Uttam Nagar
- gallbladder surgery in Uttam Nagar
- gall bladder surgery in Uttam Nagar
- best Oncologist in Hari Nagar
- best oncosurgeon in Hari Nagar
- best onco surgeon in Hari Nagar
- best gastro surgeon in Hari Nagar
- best gastro doctor in Hari Nagar
- best gastrosurgeon in Hari Nagar
- best robotic surgeon in Hari Nagar
- best robotic cancer surgeon in Hari Nagar
- best laparoscopic surgeon in Hari Nagar
- gallbladder surgery in Hari Nagar
- gall bladder surgery in Hari Nagar
- best Oncologist in Tilak Nagar
- best oncosurgeon in Tilak Nagar
- best onco surgeon in Tilak Nagar
- best gastro surgeon in Tilak Nagar
- best gastro doctor in Tilak Nagar
- best gastrosurgeon in Tilak Nagar
- best robotic surgeon in Tilak Nagar
- best robotic cancer surgeon in Tilak Nagar
- best laparoscopic surgeon in Tilak Nagar
- gallbladder surgery in Tilak Nagar
- gall bladder surgery in Tilak Nagar
- best Oncologist in Punjabi Bagh
- best oncosurgeon in Punjabi Bagh
- best onco surgeon in Punjabi Bagh
- best gastro surgeon in Punjabi Bagh
- best gastro doctor in Punjabi Bagh
- best gastrosurgeon in Punjabi Bagh
- best robotic surgeon in Punjabi Bagh
- best robotic cancer surgeon in Punjabi Bagh
- best laparoscopic surgeon in Punjabi Bagh
- gallbladder surgery in Punjabi Bagh
- gall bladder surgery in Punjabi Bagh
- best Oncologist in West Delhi
- best oncosurgeon in West Delhi
- best onco surgeon in West Delhi
- best gastro surgeon in West Delhi
- best gastro doctor in West Delhi
- best gastrosurgeon in West Delhi
- best robotic surgeon in West Delhi
- best robotic cancer surgeon in West Delhi
- best laparoscopic surgeon in West Delhi
- gallbladder surgery in West Delhi
- gall bladder surgery in West Delhi
- best Oncologist in Subhash Nagar
- best oncosurgeon in Subhash Nagar
- best onco surgeon in Subhash Nagar
- best gastro surgeon in Subhash Nagar
- best gastro doctor in Subhash Nagar
- best gastrosurgeon in Subhash Nagar
- best robotic surgeon in Subhash Nagar
- best robotic cancer surgeon in Subhash Nagar
- best laparoscopic surgeon in Subhash Nagar
- gallbladder surgery in Subhash Nagar
- gall bladder surgery in Subhash Nagar
- Cholecystectomy Treatment in Pitampura
- Pancreatic Cancer Treatment in Pitampura
- Esophageal Cancer Treatment in Pitampura
- Colorectal Cancer Treatment in Pitampura
- Gastric Cancer Treatment in Pitampura
- Gallbladder Cancer Treatment in Pitampura
- Robotic GI Surgery in Pitampura
- Laparoscopic GI Surgery in Pitampura
- Cholecystectomy Treatment in Dwarka
- Pancreatic Cancer Treatment in Dwarka
- Esophageal Cancer Treatment in Dwarka
- Colorectal Cancer Treatment in Dwarka
- Gastric Cancer Treatment in Dwarka
- Gallbladder Cancer Treatment in Dwarka
- Robotic GI Surgery in Dwarka
- Laparoscopic GI Surgery in Dwarka
- GERD Surgery in Dwarka
- Cholecystectomy Treatment in Dwarka
- GERD Surgery in Janakpuri
- Cholecystectomy Treatment in Janakpuri
- Pancreatic Cancer Treatment in Janakpuri
- Esophageal Cancer Treatment in Janakpuri
- Colorectal Cancer Treatment in Janakpuri
- Gastric Cancer Treatment in Janakpuri
- Gallbladder Cancer Treatment in Janakpuri
- Robotic GI Surgery in Janakpuri
- Laparoscopic GI Surgery in Janakpuri
- GERD Surgery in Palam
- Cholecystectomy Treatment in Palam
- Pancreatic Cancer Treatment in Palam
- Esophageal Cancer Treatment in Palam
- Colorectal Cancer Treatment in Palam
- Gastric Cancer Treatment in Palam
- Gallbladder Cancer Treatment in Palam
- Robotic GI Surgery in Palam
- Laparoscopic GI Surgery in Palam
- GERD Surgery in Najafgarh
- Cholecystectomy Treatment in Najafgarh
- Pancreatic Cancer Treatment in Najafgarh
- Esophageal Cancer Treatment in Najafgarh
- Colorectal Cancer Treatment in Najafgarh
- Gastric Cancer Treatment in Najafgarh
- Gallbladder Cancer Treatment in Najafgarh
- Robotic GI Surgery in Najafgarh
- Laparoscopic GI Surgery in Najafgarh
- GERD Surgery in Ashok Vihar
- Cholecystectomy Treatment in Ashok Vihar
- Pancreatic Cancer Treatment in Ashok Vihar
- Esophageal Cancer Treatment in Ashok Vihar
- Colorectal Cancer Treatment in Ashok Vihar
- Gastric Cancer Treatment in Ashok Vihar
- Gallbladder Cancer Treatment in Ashok Vihar
- Robotic GI Surgery in Ashok Vihar
- Laparoscopic GI Surgery in Ashok Vihar
- GERD Surgery in Shalimar Bagh
- Cholecystectomy Treatment in Shalimar Bagh
- Pancreatic Cancer Treatment in Shalimar Bagh
- Esophageal Cancer Treatment in Shalimar Bagh
- Colorectal Cancer Treatment in Shalimar Bagh
- Gastric Cancer Treatment in Shalimar Bagh
- Gallbladder Cancer Treatment in Shalimar Bagh
- Robotic GI Surgery in Shalimar Bagh
- Laparoscopic GI Surgery in Shalimar Bagh
- GERD Surgery in Rohini
- Cholecystectomy Treatment in Rohini
- Pancreatic Cancer Treatment in Rohini
- Esophageal Cancer Treatment in Rohini
- Colorectal Cancer Treatment in Rohini
- Gastric Cancer Treatment in Rohini
- Gallbladder Cancer Treatment in Rohini
- Robotic GI Surgery in Rohini
- Laparoscopic GI Surgery in Rohini
- GERD Surgery in Tilak Nagar
- Cholecystectomy Treatment in Tilak Nagar
- Pancreatic Cancer Treatment in Tilak Nagar
- Esophageal Cancer Treatment in Tilak Nagar
- Colorectal Cancer Treatment in Tilak Nagar
- Gastric Cancer Treatment in Tilak Nagar
- Gallbladder Cancer Treatment in Tilak Nagar
- Robotic GI Surgery in Tilak Nagar
- Laparoscopic GI Surgery in Tilak Nagar
- GERD Surgery in Punjabi Bagh
- Cholecystectomy Treatment in Punjabi Bagh
- Pancreatic Cancer Treatment in Punjabi Bagh
- Esophageal Cancer Treatment in Punjabi Bagh
- Colorectal Cancer Treatment in Punjabi Bagh
- Gastric Cancer Treatment in Punjabi Bagh
- Gallbladder Cancer Treatment in Punjabi Bagh
- Robotic GI Surgery in Punjabi Bagh
- Laparoscopic GI Surgery in Punjabi Bagh
- GERD Surgery in Subhash Nagar
- Cholecystectomy Treatment in Subhash Nagar
- Pancreatic Cancer Treatment in Subhash Nagar
- Esophageal Cancer Treatment in Subhash Nagar
- Colorectal Cancer Treatment in Subhash Nagar
- Gastric Cancer Treatment in Subhash Nagar
- Gallbladder Cancer Treatment in Subhash Nagar
- Robotic GI Surgery in Subhash Nagar
- Laparoscopic GI Surgery in Subhash Nagar
- GERD Surgery in West Delhi
- Cholecystectomy Treatment in West Delhi
- Pancreatic Cancer Treatment in West Delhi
- Esophageal Cancer Treatment in West Delhi
- Colorectal Cancer Treatment in West Delhi
- Gastric Cancer Treatment in West Delhi
- Gallbladder Cancer Treatment in West Delhi
- Robotic GI Surgery in West Delhi
- Laparoscopic GI Surgery in West Delhi
- Best Oncologist in Mayur Vihar
- Best Oncosurgeon in Mayur Vihar
- best gastro surgeon in Mayur Vihar
- Best Robotic Surgeon in Mayur Vihar
- Best Laparoscopic Surgeon in Mayur Vihar
- best Gallbladder Surgery in Mayur Vihar
- liver transplant surgeon in Mayur Vihar
- Best liver transplant surgeon in Mayur Vihar
- best robotic cancer surgeon in Mayur Vihar
- best laparoscopic cancer surgeon in Mayur Vihar
- best surgical gastroenterologist in Mayur Vihar
- best GI Surgery Specialist in Mayur Vihar
- GI Surgery Specialist in Mayur Vihar
- Chronic Pancreatitis Treatment Specialist in Mayur Vihar
- Surgeon for GI Surgery in Mayur Vihar
- Surgeon for sleeve gastrectomy in Mayur Vihar
- Gallbladder Removal Surgeon in Mayur Vihar
- Best Gallbladder Removal Surgeon in Mayur Vihar
- Gallbladder Removal Surgery in Mayur Vihar
- Pancreato Biliary Surgery in Mayur Vihar
- Thoracoscopic Esophageal Surgery in Mayur Vihar
- Laparoscopic Colorectal Surgery in Mayur Vihar
- best Oncologist in Mayur Vihar
- best oncosurgeon in Mayur Vihar
- best onco surgeon in Mayur Vihar
- best gastro doctor in Mayur Vihar
- best gastrosurgeon in Mayur Vihar
- best robotic surgeon in Mayur Vihar
- best laparoscopic surgeon in Mayur Vihar
- gallbladder surgery in Mayur Vihar
- gall bladder surgery in Mayur Vihar
- GERD Surgery in Mayur Vihar
- Cholecystectomy Treatment in Mayur Vihar
- Pancreatic Cancer Treatment in Mayur Vihar
- Esophageal Cancer Treatment in Mayur Vihar
- Colorectal Cancer Treatment in Mayur Vihar
- Gastric Cancer Treatment in Mayur Vihar
- Gallbladder Cancer Treatment in Mayur Vihar
- Robotic GI Surgery in Mayur Vihar
- Laparoscopic GI Surgery in Mayur Vihar
- Best Oncologist in Noida Sector 15
- Best Oncosurgeon in Noida Sector 15
- best gastro surgeon in Noida Sector 15
- Best Robotic Surgeon in Noida Sector 15
- Best Laparoscopic Surgeon in Noida Sector 15
- best Gallbladder Surgery in Noida Sector 15
- liver transplant surgeon in Noida Sector 15
- Best liver transplant surgeon in Noida Sector 15
- best robotic cancer surgeon in Noida Sector 15
- best laparoscopic cancer surgeon in Noida Sector 15
- best surgical gastroenterologist in Noida Sector 15
- best GI Surgery Specialist in Noida Sector 15
- GI Surgery Specialist in Noida Sector 15
- Chronic Pancreatitis Treatment Specialist in Noida Sector 15
- Surgeon for GI Surgery in Noida Sector 15
- Surgeon for sleeve gastrectomy in Noida Sector 15
- Gallbladder Removal Surgeon in Noida Sector 15
- Best Gallbladder Removal Surgeon in Noida Sector 15
- Gallbladder Removal Surgery in Noida Sector 15
- Pancreato Biliary Surgery in Noida Sector 15
- Thoracoscopic Esophageal Surgery in Noida Sector 15
- Laparoscopic Colorectal Surgery in Noida Sector 15
- best Oncologist in Noida Sector 15
- best oncosurgeon in Noida Sector 15
- best onco surgeon in Noida Sector 15
- best gastro doctor in Noida Sector 15
- best gastrosurgeon in Noida Sector 15
- best robotic surgeon in Noida Sector 15
- best laparoscopic surgeon in Noida Sector 15
- gallbladder surgery in Noida Sector 15
- gall bladder surgery in Noida Sector 15
- GERD Surgery in Noida Sector 15
- Cholecystectomy Treatment in Noida Sector 15
- Pancreatic Cancer Treatment in Noida Sector 15
- Esophageal Cancer Treatment in Noida Sector 15
- Colorectal Cancer Treatment in Noida Sector 15
- Gastric Cancer Treatment in Noida Sector 15
- Gallbladder Cancer Treatment in Noida Sector 15
- Robotic GI Surgery in Noida Sector 15
- Laparoscopic GI Surgery in Noida Sector 15
- Best Oncologist in Noida Sector 8
- Best Oncosurgeon in Noida Sector 8
- best gastro surgeon in Noida Sector 8
- Best Robotic Surgeon in Noida Sector 8
- Best Laparoscopic Surgeon in Noida Sector 8
- best Gallbladder Surgery in Noida Sector 8
- liver transplant surgeon in Noida Sector 8
- Best liver transplant surgeon in Noida Sector 8
- best robotic cancer surgeon in Noida Sector 8
- best laparoscopic cancer surgeon in Noida Sector 8
- best surgical gastroenterologist in Noida Sector 8
- best GI Surgery Specialist in Noida Sector 8
- GI Surgery Specialist in Noida Sector 8
- Chronic Pancreatitis Treatment Specialist in Noida Sector 8
- Surgeon for GI Surgery in Noida Sector 8
- Surgeon for sleeve gastrectomy in Noida Sector 8
- Gallbladder Removal Surgeon in Noida Sector 8
- Best Gallbladder Removal Surgeon in Noida Sector 8
- Gallbladder Removal Surgery in Noida Sector 8
- Pancreato Biliary Surgery in Noida Sector 8
- Thoracoscopic Esophageal Surgery in Noida Sector 8
- Laparoscopic Colorectal Surgery in Noida Sector 8
- best Oncologist in Noida Sector 8
- best oncosurgeon in Noida Sector 8
- best onco surgeon in Noida Sector 8
- best gastro doctor in Noida Sector 8
- best gastrosurgeon in Noida Sector 8
- best robotic surgeon in Noida Sector 8
- best laparoscopic surgeon in Noida Sector 8
- gallbladder surgery in Noida Sector 8
- gall bladder surgery in Noida Sector 8
- GERD Surgery in Noida Sector 8
- Cholecystectomy Treatment in Noida Sector 8
- Pancreatic Cancer Treatment in Noida Sector 8
- Esophageal Cancer Treatment in Noida Sector 8
- Colorectal Cancer Treatment in Noida Sector 8
- Gastric Cancer Treatment in Noida Sector 8
- Gallbladder Cancer Treatment in Noida Sector 8
- Robotic GI Surgery in Noida Sector 8
- Laparoscopic GI Surgery in Noida Sector 8
- Best Oncologist in Noida Sector 9
- Best Oncosurgeon in Noida Sector 9
- best gastro surgeon in Noida Sector 9
- Best Robotic Surgeon in Noida Sector 9
- Best Laparoscopic Surgeon in Noida Sector 9
- best Gallbladder Surgery in Noida Sector 9
- liver transplant surgeon in Noida Sector 9
- Best liver transplant surgeon in Noida Sector 9
- best robotic cancer surgeon in Noida Sector 9
- best laparoscopic cancer surgeon in Noida Sector 9
- best surgical gastroenterologist in Noida Sector 9
- best GI Surgery Specialist in Noida Sector 9
- GI Surgery Specialist in Noida Sector 9
- Chronic Pancreatitis Treatment Specialist in Noida Sector 9
- Surgeon for GI Surgery in Noida Sector 9
- Surgeon for sleeve gastrectomy in Noida Sector 9
- Gallbladder Removal Surgeon in Noida Sector 9
- Best Gallbladder Removal Surgeon in Noida Sector 9
- Gallbladder Removal Surgery in Noida Sector 9
- Pancreato Biliary Surgery in Noida Sector 9
- Thoracoscopic Esophageal Surgery in Noida Sector 9
- Laparoscopic Colorectal Surgery in Noida Sector 9
- best Oncologist in Noida Sector 9
- best oncosurgeon in Noida Sector 9
- best onco surgeon in Noida Sector 9
- best gastro doctor in Noida Sector 9
- best gastrosurgeon in Noida Sector 9
- best robotic surgeon in Noida Sector 9
- best laparoscopic surgeon in Noida Sector 9
- gallbladder surgery in Noida Sector 9
- gall bladder surgery in Noida Sector 9
- GERD Surgery in Noida Sector 9
- Cholecystectomy Treatment in Noida Sector 9
- Pancreatic Cancer Treatment in Noida Sector 9
- Esophageal Cancer Treatment in Noida Sector 9
- Colorectal Cancer Treatment in Noida Sector 9
- Gastric Cancer Treatment in Noida Sector 9
- Gallbladder Cancer Treatment in Noida Sector 9
- Robotic GI Surgery in Noida Sector 9
- Laparoscopic GI Surgery in Noida Sector 9
- Best Oncologist in Noida Sector 16
- Best Oncosurgeon in Noida Sector 16
- best gastro surgeon in Noida Sector 16
- Best Robotic Surgeon in Noida Sector 16
- Best Laparoscopic Surgeon in Noida Sector 16
- best Gallbladder Surgery in Noida Sector 16
- liver transplant surgeon in Noida Sector 16
- Best liver transplant surgeon in Noida Sector 16
- best robotic cancer surgeon in Noida Sector 16
- best laparoscopic cancer surgeon in Noida Sector 16
- best surgical gastroenterologist in Noida Sector 16
- best GI Surgery Specialist in Noida Sector 16
- GI Surgery Specialist in Noida Sector 16
- Chronic Pancreatitis Treatment Specialist in Noida Sector 16
- Surgeon for GI Surgery in Noida Sector 16
- Surgeon for sleeve gastrectomy in Noida Sector 16
- Gallbladder Removal Surgeon in Noida Sector 16
- Best Gallbladder Removal Surgeon in Noida Sector 16
- Gallbladder Removal Surgery in Noida Sector 16
- Pancreato Biliary Surgery in Noida Sector 16
- Thoracoscopic Esophageal Surgery in Noida Sector 16
- Laparoscopic Colorectal Surgery in Noida Sector 16
- best Oncologist in Noida Sector 16
- best oncosurgeon in Noida Sector 16
- best onco surgeon in Noida Sector 16
- best gastro doctor in Noida Sector 16
- best gastrosurgeon in Noida Sector 16
- best robotic surgeon in Noida Sector 16
- best laparoscopic surgeon in Noida Sector 16
- gallbladder surgery in Noida Sector 16
- gall bladder surgery in Noida Sector 16
- GERD Surgery in Noida Sector 16
- Cholecystectomy Treatment in Noida Sector 16
- Pancreatic Cancer Treatment in Noida Sector 16
- Esophageal Cancer Treatment in Noida Sector 16
- Colorectal Cancer Treatment in Noida Sector 16
- Gastric Cancer Treatment in Noida Sector 16
- Gallbladder Cancer Treatment in Noida Sector 16
- Robotic GI Surgery in Noida Sector 16
- Laparoscopic GI Surgery in Noida Sector 16
- Best Oncologist in New Ashok Nagar
- Best Oncosurgeon in New Ashok Nagar
- best gastro surgeon in New Ashok Nagar
- Best Robotic Surgeon in New Ashok Nagar
- Best Laparoscopic Surgeon in New Ashok Nagar
- best Gallbladder Surgery in New Ashok Nagar
- liver transplant surgeon in New Ashok Nagar
- Best liver transplant surgeon in New Ashok Nagar
- best robotic cancer surgeon in New Ashok Nagar
- best laparoscopic cancer surgeon in New Ashok Nagar
- best surgical gastroenterologist in New Ashok Nagar
- best GI Surgery Specialist in New Ashok Nagar
- GI Surgery Specialist in New Ashok Nagar
- Chronic Pancreatitis Treatment Specialist in New Ashok Nagar
- Surgeon for GI Surgery in New Ashok Nagar
- Surgeon for sleeve gastrectomy in New Ashok Nagar
- Gallbladder Removal Surgeon in New Ashok Nagar
- Best Gallbladder Removal Surgeon in New Ashok Nagar
- Gallbladder Removal Surgery in New Ashok Nagar
- Pancreato Biliary Surgery in New Ashok Nagar
- Thoracoscopic Esophageal Surgery in New Ashok Nagar
- Laparoscopic Colorectal Surgery in New Ashok Nagar
- best Oncologist in New Ashok Nagar
- best oncosurgeon in New Ashok Nagar
- best onco surgeon in New Ashok Nagar
- best gastro doctor in New Ashok Nagar
- best gastrosurgeon in New Ashok Nagar
- best robotic surgeon in New Ashok Nagar
- best laparoscopic surgeon in New Ashok Nagar
- gallbladder surgery in New Ashok Nagar
- gall bladder surgery in New Ashok Nagar
- GERD Surgery in New Ashok Nagar
- Cholecystectomy Treatment in New Ashok Nagar
- Pancreatic Cancer Treatment in New Ashok Nagar
- Esophageal Cancer Treatment in New Ashok Nagar
- Colorectal Cancer Treatment in New Ashok Nagar
- Gastric Cancer Treatment in New Ashok Nagar
- Gallbladder Cancer Treatment in New Ashok Nagar
- Robotic GI Surgery in New Ashok Nagar
- Laparoscopic GI Surgery in New Ashok Nagar
- Best Oncologist in Nyay Khand
- Best Oncosurgeon in Nyay Khand
- best gastro surgeon in Nyay Khand
- Best Robotic Surgeon in Nyay Khand
- Best Laparoscopic Surgeon in Nyay Khand
- best Gallbladder Surgery in Nyay Khand
- liver transplant surgeon in Nyay Khand
- Best liver transplant surgeon in Nyay Khand
- best robotic cancer surgeon in Nyay Khand
- best laparoscopic cancer surgeon in Nyay Khand
- best surgical gastroenterologist in Nyay Khand
- best GI Surgery Specialist in Nyay Khand
- GI Surgery Specialist in Nyay Khand
- Chronic Pancreatitis Treatment Specialist in Nyay Khand
- Surgeon for GI Surgery in Nyay Khand
- Surgeon for sleeve gastrectomy in Nyay Khand
- Gallbladder Removal Surgeon in Nyay Khand
- Best Gallbladder Removal Surgeon in Nyay Khand
- Gallbladder Removal Surgery in Nyay Khand
- Pancreato Biliary Surgery in Nyay Khand
- Thoracoscopic Esophageal Surgery in Nyay Khand
- Laparoscopic Colorectal Surgery in Nyay Khand
- best Oncologist in Nyay Khand
- best oncosurgeon in Nyay Khand
- best onco surgeon in Nyay Khand
- best gastro doctor in Nyay Khand
- best gastrosurgeon in Nyay Khand
- best robotic surgeon in Nyay Khand
- best laparoscopic surgeon in Nyay Khand
- gallbladder surgery in Nyay Khand
- gall bladder surgery in Nyay Khand
- GERD Surgery in Nyay Khand
- Cholecystectomy Treatment in Nyay Khand
- Pancreatic Cancer Treatment in Nyay Khand
- Esophageal Cancer Treatment in Nyay Khand
- Colorectal Cancer Treatment in Nyay Khand
- Gastric Cancer Treatment in Nyay Khand
- Gallbladder Cancer Treatment in Nyay Khand
- Robotic GI Surgery in Nyay Khand
- Laparoscopic GI Surgery in Nyay Khand
- Best Oncologist in Abhay Khand
- Best Oncosurgeon in Abhay Khand
- best gastro surgeon in Abhay Khand
- Best Robotic Surgeon in Abhay Khand
- Best Laparoscopic Surgeon in Abhay Khand
- best Gallbladder Surgery in Abhay Khand
- liver transplant surgeon in Abhay Khand
- Best liver transplant surgeon in Abhay Khand
- best robotic cancer surgeon in Abhay Khand
- best laparoscopic cancer surgeon in Abhay Khand
- best surgical gastroenterologist in Abhay Khand
- best GI Surgery Specialist in Abhay Khand
- GI Surgery Specialist in Abhay Khand
- Chronic Pancreatitis Treatment Specialist in Abhay Khand
- Surgeon for GI Surgery in Abhay Khand
- Surgeon for sleeve gastrectomy in Abhay Khand
- Gallbladder Removal Surgeon in Abhay Khand
- Best Gallbladder Removal Surgeon in Abhay Khand
- Gallbladder Removal Surgery in Abhay Khand
- Pancreato Biliary Surgery in Abhay Khand
- Thoracoscopic Esophageal Surgery in Abhay Khand
- Laparoscopic Colorectal Surgery in Abhay Khand
- best Oncologist in Abhay Khand
- best oncosurgeon in Abhay Khand
- best onco surgeon in Abhay Khand
- best gastro doctor in Abhay Khand
- best gastrosurgeon in Abhay Khand
- best robotic surgeon in Abhay Khand
- best laparoscopic surgeon in Abhay Khand
- gallbladder surgery in Abhay Khand
- gall bladder surgery in Abhay Khand
- GERD Surgery in Abhay Khand
- Cholecystectomy Treatment in Abhay Khand
- Pancreatic Cancer Treatment in Abhay Khand
- Esophageal Cancer Treatment in Abhay Khand
- Colorectal Cancer Treatment in Abhay Khand
- Gastric Cancer Treatment in Abhay Khand
- Gallbladder Cancer Treatment in Abhay Khand
- Robotic GI Surgery in Abhay Khand
- Laparoscopic GI Surgery in Abhay Khand
- Best Oncologist in Vaishali
- Best Oncosurgeon in Vaishali
- best gastro surgeon in Vaishali
- Best Robotic Surgeon in Vaishali
- Best Laparoscopic Surgeon in Vaishali
- best Gallbladder Surgery in Vaishali
- liver transplant surgeon in Vaishali
- Best liver transplant surgeon in Vaishali
- best robotic cancer surgeon in Vaishali
- best laparoscopic cancer surgeon in Vaishali
- best surgical gastroenterologist in Vaishali
- best GI Surgery Specialist in Vaishali
- GI Surgery Specialist in Vaishali
- Chronic Pancreatitis Treatment Specialist in Vaishali
- Surgeon for GI Surgery in Vaishali
- Surgeon for sleeve gastrectomy in Vaishali
- Gallbladder Removal Surgeon in Vaishali
- Best Gallbladder Removal Surgeon in Vaishali
- Gallbladder Removal Surgery in Vaishali
- Pancreato Biliary Surgery in Vaishali
- Thoracoscopic Esophageal Surgery in Vaishali
- Laparoscopic Colorectal Surgery in Vaishali
- best Oncologist in Vaishali
- best oncosurgeon in Vaishali
- best onco surgeon in Vaishali
- best gastro doctor in Vaishali
- best gastrosurgeon in Vaishali
- best robotic surgeon in Vaishali
- best laparoscopic surgeon in Vaishali
- gallbladder surgery in Vaishali
- gall bladder surgery in Vaishali
- GERD Surgery in Vaishali
- Cholecystectomy Treatment in Vaishali
- Pancreatic Cancer Treatment in Vaishali
- Esophageal Cancer Treatment in Vaishali
- Colorectal Cancer Treatment in Vaishali
- Gastric Cancer Treatment in Vaishali
- Gallbladder Cancer Treatment in Vaishali
- Robotic GI Surgery in Vaishali
- Laparoscopic GI Surgery in Vaishali
- Best Oncologist in Patparganj
- Best Oncosurgeon in Patparganj
- best gastro surgeon in Patparganj
- Best Robotic Surgeon in Patparganj
- Best Laparoscopic Surgeon in Patparganj
- best Gallbladder Surgery in Patparganj
- liver transplant surgeon in Patparganj
- Best liver transplant surgeon in Patparganj
- best robotic cancer surgeon in Patparganj
- best laparoscopic cancer surgeon in Patparganj
- best surgical gastroenterologist in Patparganj
- best GI Surgery Specialist in Patparganj
- GI Surgery Specialist in Patparganj
- Chronic Pancreatitis Treatment Specialist in Patparganj
- Surgeon for GI Surgery in Patparganj
- Surgeon for sleeve gastrectomy in Patparganj
- Gallbladder Removal Surgeon in Patparganj
- Best Gallbladder Removal Surgeon in Patparganj
- Gallbladder Removal Surgery in Patparganj
- Pancreato Biliary Surgery in Patparganj
- Thoracoscopic Esophageal Surgery in Patparganj
- Laparoscopic Colorectal Surgery in Patparganj
- best Oncologist in Patparganj
- best oncosurgeon in Patparganj
- best onco surgeon in Patparganj
- best gastro doctor in Patparganj
- best gastrosurgeon in Patparganj
- best robotic surgeon in Patparganj
- best laparoscopic surgeon in Patparganj
- gallbladder surgery in Patparganj
- gall bladder surgery in Patparganj
- GERD Surgery in Patparganj
- Cholecystectomy Treatment in Patparganj
- Pancreatic Cancer Treatment in Patparganj
- Esophageal Cancer Treatment in Patparganj
- Colorectal Cancer Treatment in Patparganj
- Gastric Cancer Treatment in Patparganj
- Gallbladder Cancer Treatment in Patparganj
- Robotic GI Surgery in Patparganj
- Laparoscopic GI Surgery in Patparganj
- Best Oncologist in IP Extension
- Best Oncosurgeon in IP Extension
- best gastro surgeon in IP Extension
- Best Robotic Surgeon in IP Extension
- Best Laparoscopic Surgeon in IP Extension
- best Gallbladder Surgery in IP Extension
- liver transplant surgeon in IP Extension
- Best liver transplant surgeon in IP Extension
- best robotic cancer surgeon in IP Extension
- best laparoscopic cancer surgeon in IP Extension
- best surgical gastroenterologist in IP Extension
- best GI Surgery Specialist in IP Extension
- GI Surgery Specialist in IP Extension
- Chronic Pancreatitis Treatment Specialist in IP Extension
- Surgeon for GI Surgery in IP Extension
- Surgeon for sleeve gastrectomy in IP Extension
- Gallbladder Removal Surgeon in IP Extension
- Best Gallbladder Removal Surgeon in IP Extension
- Gallbladder Removal Surgery in IP Extension
- Pancreato Biliary Surgery in IP Extension
- Thoracoscopic Esophageal Surgery in IP Extension
- Laparoscopic Colorectal Surgery in IP Extension
- best Oncologist in IP Extension
- best oncosurgeon in IP Extension
- best onco surgeon in IP Extension
- best gastro doctor in IP Extension
- best gastrosurgeon in IP Extension
- best robotic surgeon in IP Extension
- best laparoscopic surgeon in IP Extension
- gallbladder surgery in IP Extension
- gall bladder surgery in IP Extension
- GERD Surgery in IP Extension
- Cholecystectomy Treatment in IP Extension
- Pancreatic Cancer Treatment in IP Extension
- Esophageal Cancer Treatment in IP Extension
- Colorectal Cancer Treatment in IP Extension
- Gastric Cancer Treatment in IP Extension
- Gallbladder Cancer Treatment in IP Extension
- Robotic GI Surgery in IP Extension
- Laparoscopic GI Surgery in IP Extension
- Best Oncologist in Vasundhra
- Best Oncologist in noida
- show more
- show less








